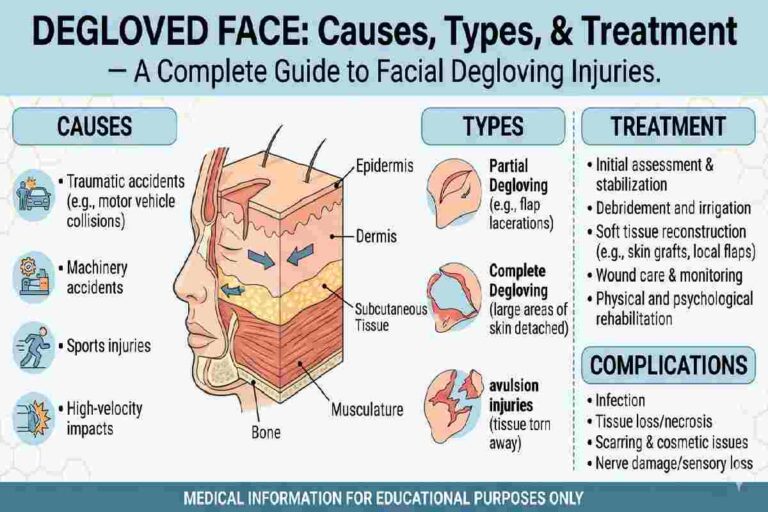
Degloved Face Causes, Types & Treatment. Degloved face- describes a serious/rare injury in which the skin and soft tissue have been forcibly removed from the face and is detached from the face‘s muscle/bone. Caused by high-energy trauma, i.e., vehicular accident/animal attack/machinery has a risk of damaging the face‘s blood vessels/muscles and bones. The face normally requires emergency surgery, tissue revision, and function restoration.
Table of Contents
What is a Degloved Face Injury?
Facial degloving, or Facial degloving injury, is the gross traumatic avulsion of skin and soft tissue (possibly including muscle) from the facial skeleton (skull, jaw, nose, and cheekbones), exposing the underlying tissue such as nerves, muscle, connective tissue, tendons, or bone. Though extremely rare.
This injury is much more catastrophic when it occurs to the face compared to a degloving injury to the limbs. The wound is distinguished by
- Severe disfigurement
- Loss of facial function (expression, chewing, vision protection)
- Psychological trauma
- High infection/necrosis risk
Search Intent Analysis
| Intent Type | Detail | What Users Want |
| Informational (90%) | Primary intent | Understand causes, types, and symptoms |
| Medical Decision | Secondary intent | Know treatment options & recovery timeline |
| Emergency | Immediate need | Recognize severity, seek urgent care |
| Commercial (10%) | Minor intent | Find specialists, hospitals, and surgeons |
User’s Problem: Seeking emergency information about severe facial trauma after an accident OR researching for medical/legal purposes.
Action User Wants: Understand severity, treatment options, recovery prognosis, and when to seek help.
Competitor & SERP Gap Analysis
What Top Competitors Cover Well
| Source | Strengths |
| WebMD () | Clear definitions, open vs. closed treatment options |
| Healthline () | Treatment options, hospital stay duration, PT needs |
| Tampa General Hospital () | Causes list, symptoms overview |
| Sancheti Hospital () | Risk factors, industrial accident causes |
Critical Gaps Identified
| Missing Content | Why It Matters |
| Facial-specific degloving detail | Most content focuses on limbs (arms/legs) |
| Hemifacial/midfacial subtypes | Rare but crucial distinctions |
| Surgical techniques (Moreau approach, MFD) | Advanced reconstruction details missing |
| India-specific data | Limited regional prevalence, cost info |
| Psychological recovery | Mental health impact often ignored |
| Case studies (real patient outcomes) | Evidence from recent medical literature |
| Recovery timeline breakdown | Week-by-week progression unclear |
Opportunity for Differentiation
This guide provides:
- Facial-specific, comprehensive detail (vs. limb-focused competitors)
- Hemifacial vs. midfacial subtype comparison
- Modern surgical approaches(scarless MFD technique)
- 2024-2025 case reports with patient outcomes
- Recovery timeline with realistic expectations
Types of Facial Degloving Injuries.
Facial degloving injuries involve shearing force that degloves skin and soft tissue from the underlying bone/muscles/fascia, as a result of a traumatic incident.
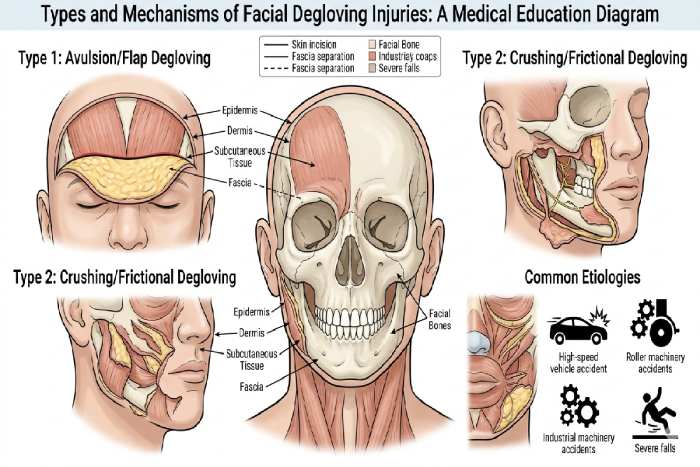
Main types of Facial Degloving injuries:
Main categories can be divided into: open and closed degloving.
The signs associated with closed degloving injury are edema, ecchymosis, tenderness, pain, and a feeling of fluctuation under the skin. Soft tissue viability is assessed by evaluating the skin’s color, temperature, capillary refill, and any bleeding.
While these variables are not a truly objective measure of true tissue viability, they do assist with treatment management decisions.
Other forms of classifying facial degloving:
Based on severity, some literature may also describe the following;
- Partial degloving: occurs when there is detachment of some layers of the soft tissue.
- Complete degloving: a complete circular degloving, affecting the whole circumference of any area, such as the limbs or face.
The facial degloving is a surgical emergency; the management is paramount to avoid necrosis and infection, especially considering the complexity of reconstructing the facial structures.
How is degloving diagnosed?
Diagnosis rests upon history and clinical examination, and appropriate imaging is dependent on open or closed degloving; closed injury typically requires complex imaging.
Clinical Assessment
Physical Examination: In physical examination, the physician seeks any noticeable findings like exposed bone and muscles, which are evident in open degloving injury.
In the presence of closed degloving injury, we would expect to find swelling, ecchymosis, tenderness, pain, and fluctuance deep under the skin. Soft tissue viability can be evaluated using the appearance, temperature, capillary refill, and the degree of bleeding of the skin. This is a crude but valuable means of deciding management:
An initial survey is carried out looking for other life-threatening injuries, and then an assessment of the extent of injury is done.
Imaging Techniques
MRI is considered the study of choice in the setting of closed degloving (e.g. Morel-Lavalle lesions) as it clearly outlines the collection of fluid and separation of tissues not apparent on inspection.
Ultrasound and CT are also used, identified by soft tissue swelling or fluctuant areas, typically when MRI is not readily available.
Plain radiographs are utilized in identifying concomitant bony injury, with clinical photos and base-line labs used to assist in planning of surgical management.
How is a degloving injury treated?
Degloving injuries are a life-threatening problem and must be treated urgently to promote healing, prevent infection, salvage tissue, and maximize functional return. Management is divided into closed and open wounds and is approached differently in each type.
Open Degloving Treatment
Prompt investigation and surgical management of the wound should be done. After initial evaluation, wound debridement should be done, removing all foreign matter, contamination, and necrotic tissue. Reattachment of degloved skin, if viable and vascular, skin grafting (flaps, muscle flap, or free graft (using NPWT usually), and finally amputation or reattachment of the digit in case of severe degloving should be considered. Broad-spectrum antibiotics and fluid resuscitation, together with close monitoring is usually started perioperatively.
Closed Degloving Treatment
Conservative options like compression bandages and physical therapy suffice for small lesions, aiding natural adhesion.
Larger Morel-Lavallée lesions need percutaneous aspiration or catheter drainage of fluid, sclerotherapy to scar the space closed, or open surgery with debridement and quilting sutures if persistent.
What is the recovery time after degloving treatment?
The healing time will differ in all patients, depending on how bad the damage is, what areas were injured (if the face, for instance), how it was treated and on how old and healthy the patient is.
Factors Affecting Timeline
Minor injuries may heal in weeks with conservative treatment, but injuries with multiple surgeries and reconstruction can take months to years to recover.
Open degloving results in longer recuperation as there is debridement, a greater chance of grafts and infection, initially ranging in hospital stay from days to weeks.
Closed injuries resolve more rapidly if the fluid is evacuated early but persistent fluid collection increases the duration of treatment.
Rehabilitation Phases
The time to initial healing and wound closure is approximately 2-8 weeks. Physiotherapy can be offered three or more times a week for restoring of function, power and movement. This, along with rehabilitation and occupational therapy, may take a matter of months, with full return to health taking 6-12 months or more in complex facial reconstructions. A side effect to long term this treatment can include scarring and lack of sensation or loss of function, which may mean a regular follow-up is necessary.
Conclusion
De-gloving injuries of the face are a serious form of trauma that demands early diagnosis with a thorough clinical evaluation and imaging studies, such as magnetic resonance imaging, and comprehensive treatment, ranging from debridement of tissues, florid or digital reconstruction. The repairs may last for weeks to over a year. The appreciation of these injuries involves a team effort and aims to reduce the complications associated with such as infection or scarring.